No laughing matter: leadership critical to help address NHS retention crisis
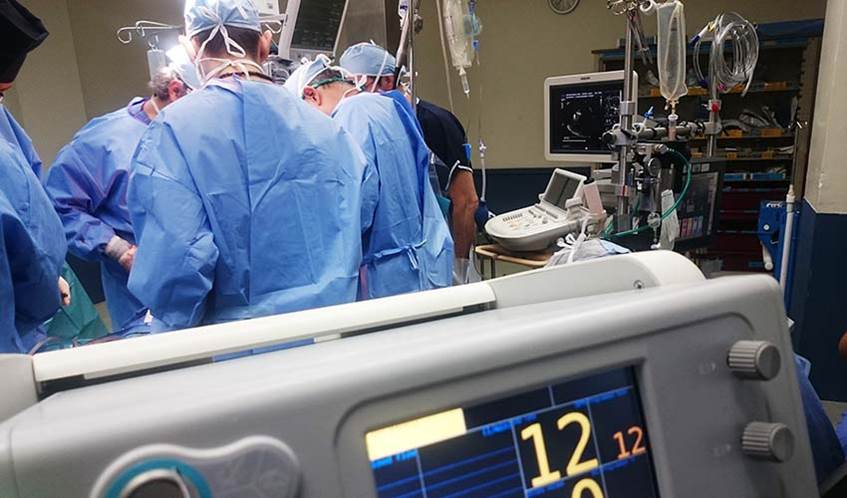
Doctors turned comedians Adam Kay, Harry Hill and Phil Hammond have teamed up with universities and the Royal College of Emergency Medicine to highlight issues underscoring the NHS retention crisis.
They were part of new research into the impact of under-resourced and high-pressure emergency hospital departments in the UK which found that frontline workers feel that they are “just rearranging the deckchairs on the Titanic”.
A study from the Royal College of Emergency Medicine and University of Bath, in collaboration with colleagues at UWE Bristol and the University of Bristol, argues that hospitals need better leadership to help change cultures and support people’s basic needs.
In addition to reflections from current frontline doctors, nurses and advanced clinical practitioners, the research features exclusive interviews with household names in the UK: former doctors turned comedians. Adam Kay, Harry Hill and Phil Hammond all offer reflections on why they left, and how they hope the NHS can be better managed in the future to avoid others from doing likewise.
In February 2023 a report concluded that as many as one in seven healthcare workers were actively trying to leave the NHS. According to the Royal College of Nursing, almost 27,000 people left the register in the past year, with more than half leaving earlier than planned citing burnout, workload, and concerns over care quality.
The new study, funded by UKRI and published in the Emergency Medicine Journal, investigated perceived barriers to implementing better working practices and conditions for emergency medicine clinicians in the UK.
Building on previous work looking at the toll of Covid for healthcare workers, its analysis highlights multiple issues associated with poor retention. These include a culture of blame and negativity in hospitals, untenable working environments, compromised leadership, as well as a perceived general lack of support leading to burnout and low morale.
Across the board, participants reported feeling undervalued due to their basic demands being unmet. These ranged from ‘sharing toilets with patients’, to poorly functioning IT systems, or the absence of rest spaces and staff rooms. A lack of private space within hospitals meant many also found it hard to decompress.
In an accompanying video to the research, comedian and former doctor Adam Kay describes a toxic culture where it was a ‘a badge of honour to work as hard as possible’, where staff felt blamed, disempowered to seek support as they should be ‘unbreakable’, and where expectations set were unrealistic.
A lack of formal training for consultants in charge of busy wards was also highlighted by a number of participants, as was the need for more ‘visible, compassionate leadership.’ Reflections from people interviewed suggested leadership training should be embedded as part of medical training.
Phil Hammond said: “We need to say to doctors, one really interesting career pathway for you is to get involved in NHS management and clinical leadership. And not in a way that says 'we have gone over to the dark side'.”
Dr Elizabeth Jenkinson, Associate Professor of Health Psychology at UWE Bristol, was co-author of the academic paper and the associated recommendations report. She provided expertise in health psychology and qualitative methods for the research.
Dr Jenkinson said: “Understanding the views of emergency medicine staff, in their own words, on what might improve their working conditions and encourage them to remain in the NHS has allowed us to develop key recommendations with the Royal College of Emergency Medicine. We hope these will have a positive impact on future working practices and workplace culture.”
Lead author Dr Jo Daniels of the University of Bath explained: “At a time of national crisis in the NHS, with over-stretched resources leading to long waiting times for patients and burnout for staff, our study asked what more could be done to improve the current challenges of staff retention.
“A common thread that emerged across our interviews was the critical importance of leadership in hospitals. Those in leadership positions are powerful agents of change, and have pivotal influence over team functioning, staff wellbeing and patient outcomes. However, lines of accountability and communication with executive management needs to be clarified, opened up and improved.
“A new focus on leadership training and ongoing support for those in leadership roles will be critical to this. Given its central importance and the scope for leadership improving wellbeing at work, we have a prime opportunity now to address the problems which force staff to leave the workforce. Harnessing the potential in our leaders is where our focus should now lie.”
To access the research Perceived barriers and opportunities to improve working conditions and staff retention in emergency departments: a qualitative study published in the Emergency Medicine Journal see https://dx.doi.org/10.1136/emermed-2023-213189
To watch interviews with Harry Hill, Phil Hammond and Adam Kay see www.bath.ac.uk/case-studies/we-are-just-rearranging-the-deckchairs-on-the-titanic/.
Related news

12 December 2025
UWE Bristol’s environmentally conscious and student-focused accommodation wins three awards
Purdown View, the world's largest certified Passivhaus student accommodation development, has been recognised at Property Week Student Accommodation Awards.

13 November 2025
Alliance Medical and UWE Bristol launch UK’s first PET-CT postgraduate certificate
In a move set to transform imaging education, Alliance Medical (AML) and UWE Bristol have joined forces to co-design and develop the UK’s first PET-CT Postgraduate Certificate (PG Cert).

10 November 2025
Lessons from Low Traffic Neighbourhoods will drive better public engagement, study finds
Lessons from Low Traffic Neighbourhoods have informed a new toolkit to improve engagement with the public on challenging local street issues.

29 September 2025
Smartphone use hitting struggling pupils hardest, major study finds
Young people struggling with their studies at school are much more likely to have negative experiences on their smartphones than their better performing peers, a major new study has found.

11 September 2025
New study to investigate augmented reality as an intervention for emotionally based school avoidance
A UWE Bristol researcher will support a new study exploring whether an augmented reality board game can help young people with emotionally based school avoidance (EBSA).

28 July 2025
Student wins bronze medal at World Aquatics Championships on her graduation day
UWE Bristol sports rehabilitation student Izzy Thorpe made waves at the World Aquatics Championships winning a bronze medal in artistic swimming on the same day she was meant to be crossing the stage at her university graduation ceremony.

28 May 2025
Leading organisations fighting to end youth violence in cities join UWE Bristol event panel
Leaders from Bristol-based Empire Fighting Chance and Canadian non-profit REACH will speak at the next Bristol Distinguished Address Series.

09 May 2025
UWE Bristol among first universities in UK to introduce sanitary waste bins in male toilets
UWE Bristol is among the first universities in the UK to introduce sanitary waste bins in male toilets for the disposal of incontinence products.

11 April 2025
UWE Bristol academics among emerging scientific leaders to receive share of £7.6m for health research
Two UWE Bristol researchers are among the recipients of a £7.6 million investment from the Academy of Medical Sciences aimed at tackling urgent health challenges.

09 April 2025
New research to support a thriving health and care workforce is launched
A national research partnership will explore ways to support wellbeing and sustainability in the NHS and social care same day and urgent care workforce.

10 March 2025
UWE Bristol to explore the power of open water swimming at upcoming event with The Wave founder Nick Hounsfield
An inspiring tale of grit and resilience will be told to audiences at the first BDAS event of 2025 as UWE Bristol welcomes Nick Hounsfield, founder of The Wave.

28 February 2025
Paramedics in GP surgeries may ease workload but not NHS costs, study finds
Paramedics working in GP surgeries help reduce GP workload but do not contribute to cost savings to the NHS, according to the first major study of the clinical and cost-effectiveness of paramedic compared with GP consultations.
You may also be interested in

Media enquiries
Enquiries related to news releases and press and contacts for the media team.

Find an expert
Media contacts are invited to check out the vast range of subjects where UWE Bristol can offer up expert commentary.
College of Health, Science and Society
The College of Health, Science and Society is a large, diverse and dynamic part of the University, bringing together experts from Health and Social Wellbeing, Applied Sciences, Education and Social Sciences






